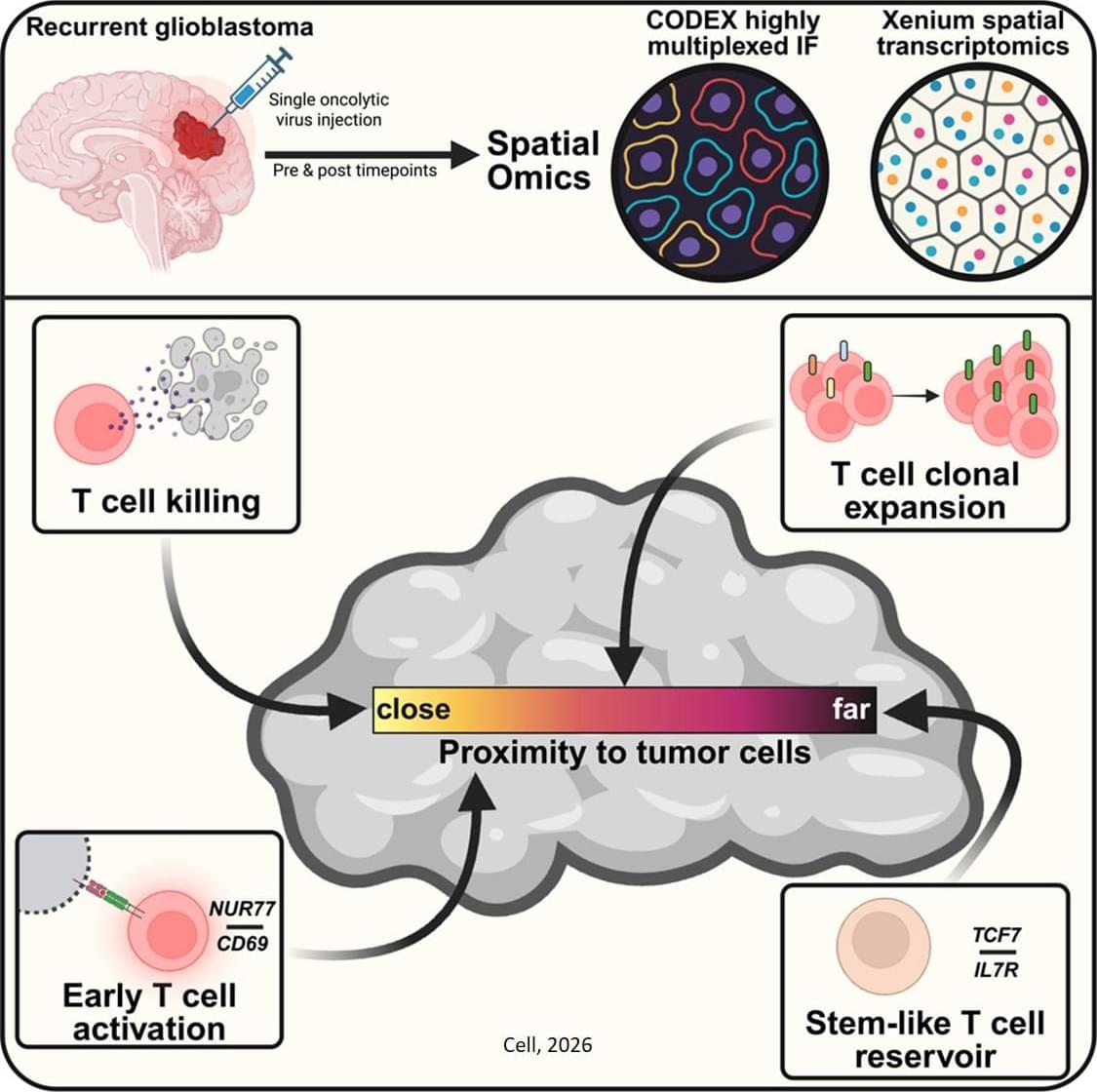
A team led by investigators has shown that a single injection of an oncolytic virus—a genetically modified virus that selectively infects and destroys cancer cells—can recruit immune cells to penetrate and persist deep within brain tumors. The research, which is published in Cell, provides details on how this therapy prolonged survival in patients with glioblastoma, the most common and malignant primary brain tumor, in a recent clinical trial.
The oncolytic virus used in the team’s trial is made from a herpes simplex virus genetically altered so it can only make copies of itself in glioblastoma cells and not normal healthy cells. The virus spreads to a glioblastoma cell, kills it, and then makes a copy of itself that spreads again to another glioblastoma cell. Infection of cells with the virus also triggers an immune response. In the phase 1 trial of 41 patients with recurrent glioblastoma, the oncolytic virus treatment extended survival compared to historically reported survival, especially among those with pre-existing viral antibodies.
In their Cell study, the investigators examined the extent of this immune response in clinical trial participants. Their analysis revealed that the treatment induced long-term infiltration of immune T cells into patients’ tumors. Closer proximity of cytotoxic T cells with dying brain tumor cells was associated with longer patient survival after treatment. The therapy also expanded pre-existing T cells in the brain. ScienceMission sciencenewshighlights.