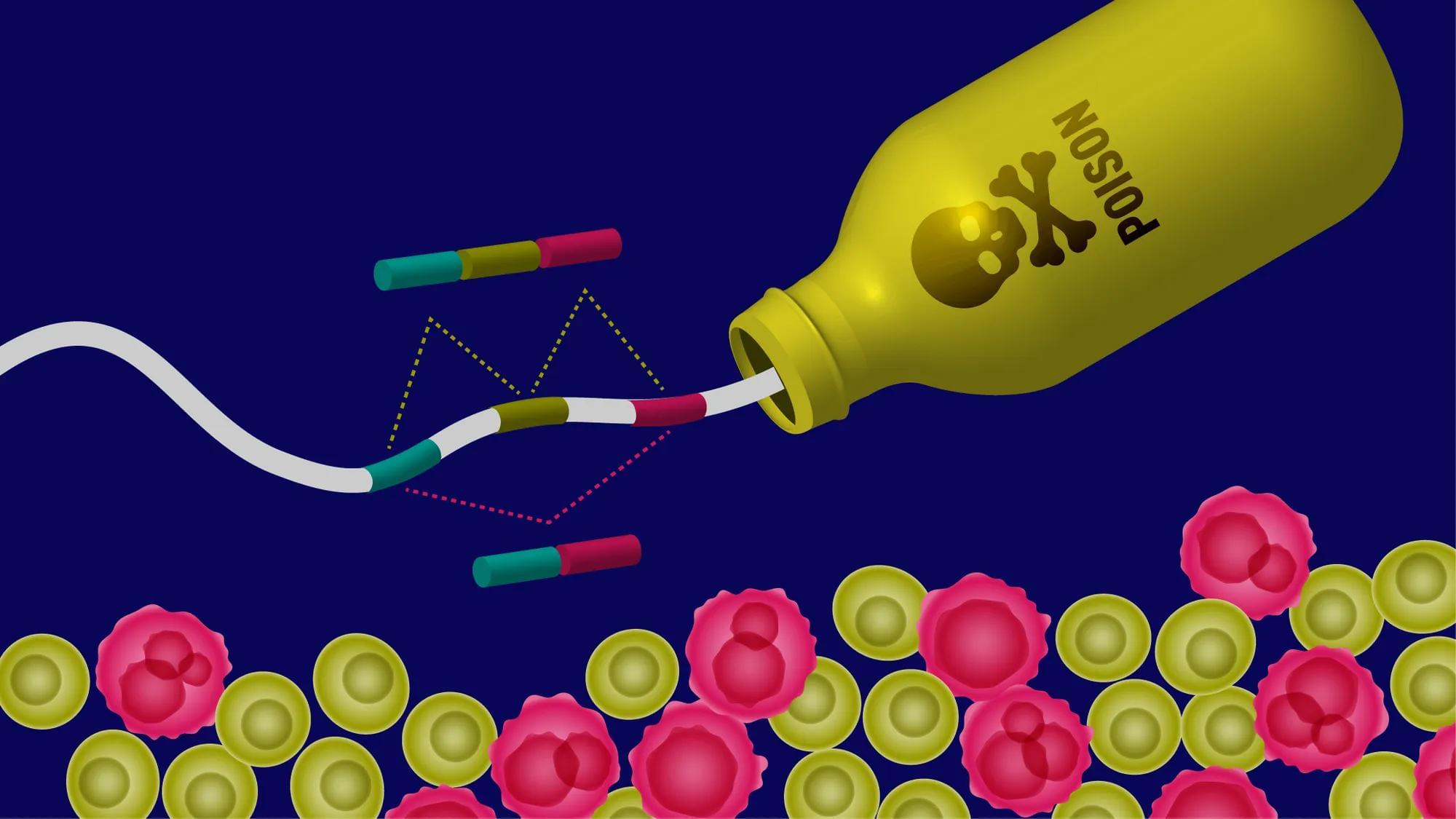
(Farmington, Conn. – March 13, 2025) – Alternative RNA splicing is like a movie editor cutting and rearranging scenes from the same footage to create different versions of a film. By selecting which scenes to keep and which to leave out, the editor can produce a drama, a comedy, or even a thriller—all from the same raw material. Similarly, cells splice RNA in different ways to produce a variety of proteins from a single gene, fine-tuning their function based on need. However, when cancer rewrites the script, this process goes awry, fueling tumor growth and survival.
In a recent study reported in the Feb. 15 issue of Nature Communications, scientists from The Jackson Laboratory (JAX) and UConn Health not only show how cancer hijacks this tightly regulated splicing and rearranging of RNA but also introduce a potential therapeutic strategy that could slow or even shrink aggressive and hard-to-treat tumors. This discovery could transform how we treat aggressive cancers like triple-negative breast cancer and certain brain tumors, where current treatment options are limited.
At the heart of this work, led by Olga Anczuków, an associate professor at JAX and co-program leader at the NCI-designated JAX Cancer Center, are tiny genetic elements called poison exons, nature’s own “off switch” for protein production. When these exons are included in an RNA message, they trigger its destruction before a protein can be made—preventing harmful cellular activity. In healthy cells, poison exons regulate the levels of key proteins, keeping the genetic machinery in check. But in cancer, this safety mechanism often fails.